The Voice
Lung Cancer Early Detection: Expanded Screening
I met an old friend for dinner recently. She got comfortable in her chair, tucked her purse under the table and ordered a tea when the waitress passed by. Mindy (not her real name) is very petite, short curly hair, quiet and health conscious since childhood. Her mother and father were committed to macrobiotics, a plant-based diet and lifestyle that aims to help people live their best physical, mental and spiritual lives. Ironically, they would chain smoke while grinding their own peanut butter at home. My friend said her family was passionate about eating food that was grown locally and in season, yet rode in a smoke-filled car with the windows rolled up as they drove out to an organic farm where you could pick your own vegetables. The smoking was such a crazy contradiction to their healthy diet, but it was the 70’s. Health consciousness followed Mindy into adulthood as did the shadow of the smoke she grew up around. She had been a smoker herself, for a couple of years as a teenager. She quit when she was pregnant with her first child and never started up again. She and her husband continued the healthy lifestyle she felt so committed to. While I knew this story from early on in our friendship, it came up again when she said she was so angry to have followed someone into the restaurant who had been smoking, blowing smoke she had to walk through and then throwing the butt into the parking lot.
The waitress set tea on the table, and we talked about our day. Mindy said she’d just had a frustrating conversation with her doctor during her annual check-up that afternoon. She started by reminding her doctor that both of her parents, an aunt, and one grandparent passed away from lung cancer. Mindy said she told him she was worrying, because she and her brother were raised from birth in a house filled with secondhand smoke. She told her doctor that she had a friend, me, who was working with Upstage Lung Cancer, and she wanted to have a referral for a baseline low dose CT scan, now that she was forty-five. Her doctor said that as a non-smoker she did not qualify as high risk according to The U.S. Preventive Services Task Force (USPSTF) guidelines. Mindy didn’t know much about the current guidelines for screening, but she had intimate knowledge of how lung cancer can be found far too late. She also knew she had some compelling risk factors that did not fit into current screening guidelines. Mindy told me she was determined to have a baseline scan, even pay out of pocket if she had to. Currently folks like my friend Mindy and others who may have genetic or environmental risk factors must advocate to receive LDCT screening, or pay out of pocket.
Need for Early Detection
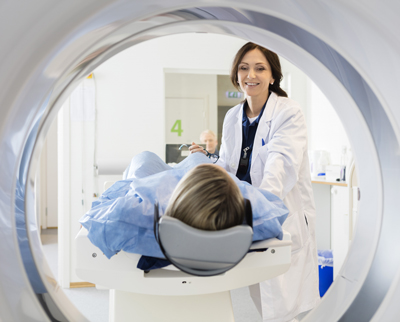
For all cancers, early detection is vital to better healthcare outcomes. Currently, screening for lung cancer is only by low dose CT scans. While an x-ray can show larger tumors, a low-dose computed tomography (also called a low-dose CT scan) shows a three-dimensional image put together by the computer combining multiple images taken by a CT machine. Possible tumors are able to be identified at greatly reduced size and with far greater accuracy compared to a standard Xray. Over the past decade the use of LDCT screening has allowed for significant progress in treatment. Early-stage detection of lung cancer is when the disease is most treatable, and those who qualify would benefit from regular screening. If found early, survival almost triples.
As of February, 2022, the Centers for Medicare & Medicaid Services (CMS) announced a national coverage determination (NCD) that expands coverage for lung cancer screening with low dose computed tomography (LDCT) to improve health outcomes for people with lung cancer. Major changes include
- Lowering the starting age from 55 to 50 years
- Extending the age for screening from 77 to 80
- Reducing the tobacco smoking history from at least 30 packs per year to at least 20 packs per year.
My friend Mindy is a determined person with means. I have no doubt she will get her needs met. Yet, there are many people in the underserved populations and people without adequate access to accurate information who will not yet receive the attention they need.
The expanded scanning criteria allows for greater access to imaging and insurance coverage for more patients who are at risk. However, GREATER EFFORTS ARE NEEDED TO BE MORE INCLUSIVE FOR THOSE WHO WANT AND NEED A SCAN.
Most insurance plans and Medicare help pay for patients who qualify for lung cancer screening tests. Check with your insurance plan to find out what benefits are covered for lung cancer screening. For more information about Medicare coverage, visit medicare.gov or call 1-800-MEDICARE (1-800-633-4227).
For additional resources visit:
Lung Cancer Screening Facts & Figures – GO2 Foundation